When the Cure’s the Cause
All the tests came back clear—but something was very wrong

As told to Faigy Peritzman
I’M a pretty busy person and getting sick doesn’t fit into my schedule. As a working mother of young children, even when I’m under the weather, I try to keep going.
Five years ago, something inside my nose began hurting me. I went to a dermatologist who prescribed a topical cream, but the pain didn’t go away. I then visited an ENT who diagnosed it as an inflamed hair follicle. That sounded pretty funny to me, but the doctor said a lot of people experience it, and it’s not a big deal. He prescribed Bactrim and told me to take it for a week. That was on a Monday.
On Thursday night, I started feeling unwell, and by Friday, I was extremely tired. But my sister was making a bar mitzvah out of town, so I packed up the whole family and went to join the simchah. Although it was fall and the weather was warm, I was freezing cold and was really not feeling well. Friday night, I left the bar mitzvah early and went to bed; I felt so lousy. During the night, I developed a high fever and could barely function. Since I wasn’t at home, I had no access to food or drink, and I became severely dehydrated.
On Motzaei Shabbos, I returned home and went to urgent care. I was so weak, still wearing a robe and lying on a bench while waiting my turn. They performed a finger prick and found that my white blood cell count was very high, but not high enough for the emergency room. They advised me to go home and follow up with my doctor the next day.
On Sunday morning, I started throwing up and couldn’t stop. Hatzalah brought me to our local ER where I received fluids. My potassium level was low, but still they couldn’t find anything majorly wrong and once I was hydrated they sent me home. And still… I continued taking my Bactrim.
My mother, who lives out of town, was supposed to fly back that day after the bar mitzvah, but my husband called her after she’d already checked in at the airport and asked her to stay and take care of me — and my family! I did feel somewhat better now that I was no longer dehydrated, but that night the fever got worse and I started experiencing intense headaches. It felt like someone was banging into my head with sledgehammers. I became hot, then freezing cold, turning on the AC and then the heating. My symptoms got so bad I called Hatzalah again, who told me to go to a larger hospital a bit further away.
At the ER, they were sure I had a contagious infection and placed me in isolation in the emergency room. It was a major perk to have some privacy, although it was very frightening to know they thought my illness warranted that!
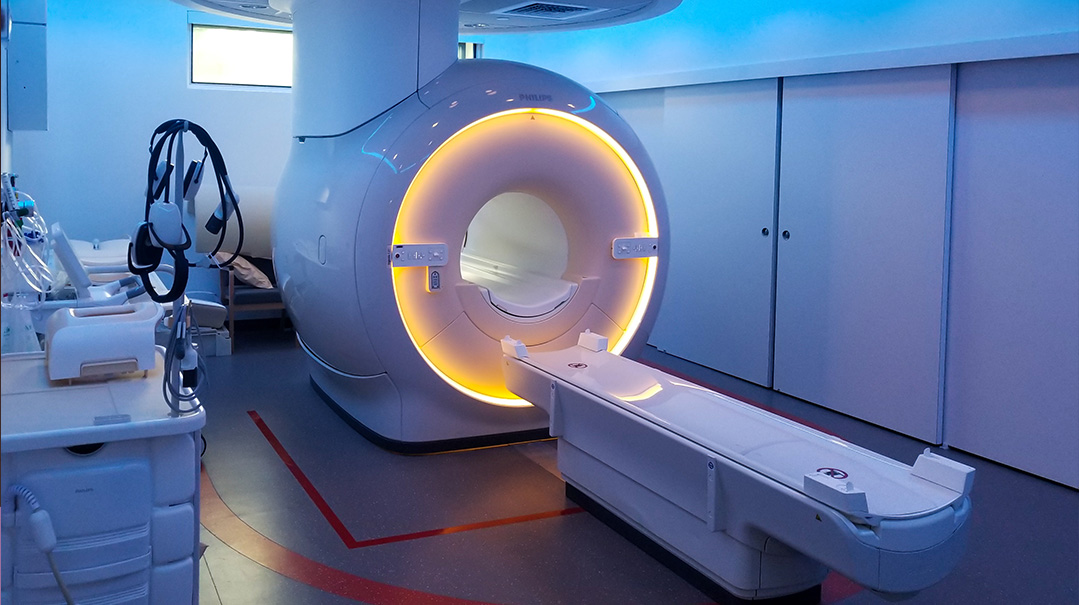
The hospital was concerned about the possibility of meningitis due to my severe headache and high fever. They performed a CT scan, an MRI, and a spinal tap — wow, that wasn’t comfortable!
But everything came out fine. However, since they didn’t know what was wrong with me, they admitted me. Throughout the week they kept drawing more and more blood for tests. At one point, my white blood cell count became so low that they told me I was a danger to myself because my immune system was suppressed, so I was switched to a private room for my own safety.
Then I developed a rash from head to toe. My face swelled up like a basketball. I had a whole team of doctors assigned to me, including a Syrian doctor and an Italian doctor. I felt like I was running my own private UN. They were all busy ruling out any possibility of diseases, which included Lyme disease, West Nile virus, and the like.
By the end of the week, I started to feel better. I had finished my regimen of Bactrim Sunday morning when I’d entered the ER and it had finally cleared from my system. Based on the way I recuperated, and the fact that all the tests for disease were negative, the doctors concluded I’d experienced a rare but severe allergic reaction to the much-prescribed Bactrim — which I’d continued like a good girl the entire time I had been so sick!
However, the staff wasn’t willing to concede this diagnosis without ruling out every other possibility. Despite feeling much better, I spent a whole week in the hospital while they ran batteries of tests. By the time I left the hospital, I’d lost ten pounds and was so weak. I’d also lost so much muscle tone from being sick and bedridden for almost two weeks that I couldn’t walk for a full week after being discharged.
But thankfully I didn’t feel sick anymore.
I was shocked to realize that an allergic reaction could have produced such a severe reaction that if I’d continued the Bactrim further, I could have died. I’ve since updated my medical records to make sure every doctor and pharmacy knows that I have a rare but severe reaction to Bactrim. For those with allergic reactions to medications, an ounce of prevention is worth a pound of those cures!
Did you ever have a medical problem that you were told “is nothing to worry about,” and it ended up being a serious issue? Did you have symptoms that stymied doctors? We believe sharing our journeys can bring awareness, empathy, and a sense of connection to those who’ve gone through a medical crisis. If you had a medical mystery and would like to be part of this column, please send a brief description of your story to familyfirst@mishpacha.com
What is a
Bactrim Allergy?
Bactrim is a sulfa-based medication used to treat things like urinary tract infections (UTIs) and skin infections. However, about three to eight percent of people are allergic to it. The reaction can cause a rash or fever in some people and more serious symptoms — including anaphylaxis — in others.
Sulfa antibiotics have been widely used for more than 70 years. These drugs even include some types of burn creams, suppositories, and eye drops. If you’ve had an allergic reaction to one sulfa antibiotic, you’re probably allergic to all of them.
Some common examples of sulfa drugs include:
Sulfamethoxazole / trimethoprim (Bactrim, Sulfatrim)
Sulfacetamide (BLEPH-10), eye drops
Sulfadiazine silver (Silvadene), burn cream
Sulfasalazine (Azulfidine), pills for rheumatoid arthritis and inflammatory bowel disease
Dapsone (Aczone), which treats leprosy, dermatitis, and certain kinds of pneumonia
Signs and Symptoms
Skin rash or hives
Itchy eyes or itchy skin
Fever
Difficulty breathing
Headaches
Insomnia
Cloudy urine
Low blood counts
Face swelling
Red or swollen skin patches that form in 30 minutes to eight hours.
Stevens-Johnson syndrome: this is a potentially life-threatening reaction that causes the skin to blister and peel off.
Anaphylaxis: This is a rare but life-threatening reaction to a drug allergy which causes trouble breathing, a drop in blood pressure, and other symptoms.
Allergy Treatments
Medications for a sulfa allergy include:
Antihistamines
Corticosteroids
Epinephrine (for anaphylaxis)
If you have a drug allergy, notify your health care providers so they can be aware of any medication that contains these allergens. Make sure these allergies are noted in your medical records. Wear a medical bracelet so that in an emergency, a bracelet will alert health care providers about any drug allergies.
Information from WebMed.com
(Originally featured in Family First, Issue 864)
Oops! We could not locate your form.