Let My Daughter Go

As the legal battle for Alta Fixsler’s life runs out of road, her father pleads for her virtual imprisonment to end
Deep into an English summer, the skies over Manchester’s Royal Children’s Hospital are that telltale pale blue holding a threat of sudden showers that means it’s August in this part of the country.
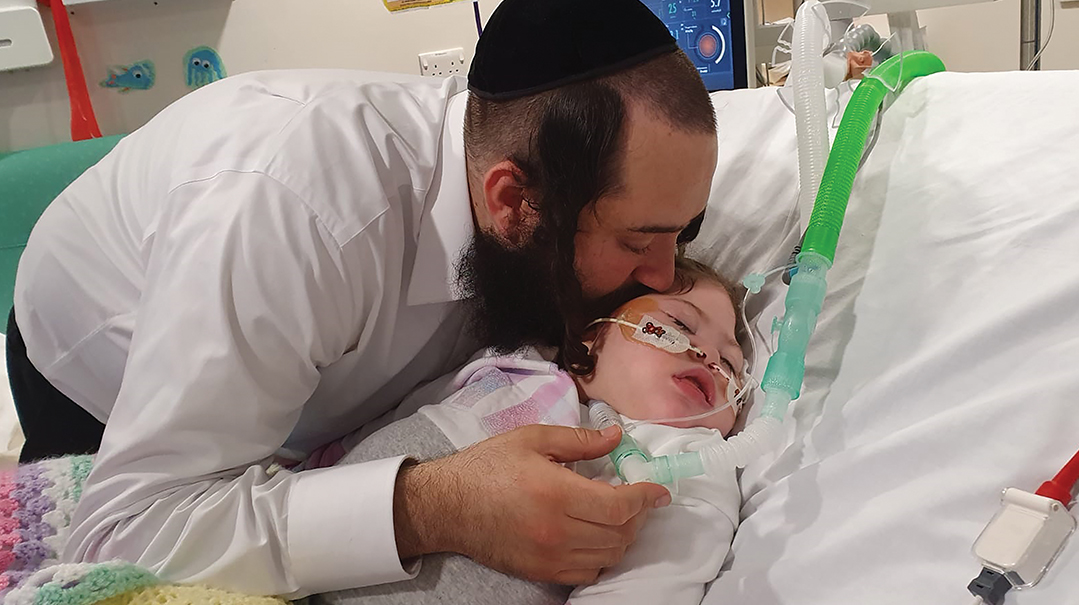
But for Alta Fixsler, a little girl lying in a windowless room inside the hospital, there’s been no summer.
Since she entered the world, Alta has only known the cold sterile walls of a hospital ward and the winter of intensive medical care. And as her family desperately fight for her survival, the British sky — so often grey and rainy — seems to cry for the fate of this child.
When little Alta was born to a chassidic family in Manchester, UK, two and a half years ago, she joined a growing list of British children who have become tragic household names due to their parents’ battle to keep them alive against the wishes of the local medical system.
Born with severe brain damage, Alta was initially declared brain-dead by doctors, who urged the parents to end their baby’s life. “They told us, ‘You’re both young — why suffer so long?’ ” recalls her father, Avraham Fixsler. “But I answered, ‘We love her as she is, and we won’t do anything to end her life earlier.’ ”
That clash of values set the stage for a battle with Britain’s National Health Service (NHS). The hospital has vowed to disconnect the sweet-faced toddler from her ventilator due to what they say is her incurable pain — an assessment Alta’s family rejects.
Almost as soon as it broke, the Alta Fixsler case drew comparisons to that of Charlie Gard and Alfie Evans, British toddlers who sparked recent end-of-life court battles. In both of those cases, the NHS refused to discharge the children for experimental treatment overseas, arguing that they had no chance of recovering and thus palliative care was the most ethical option. Then as now, British authorities were adamant that doctors, not the parents, were best suited to determine what was a humane end for these children.
So even as the case has become a fixture on frum news sites and international media over the last few months, and politicians such as US Senate Majority Leader Chuck Schumer have called on British authorities to let Alta’s parents transfer her to America or Israel, the story raises disturbing questions about Britain’s medical and legal environment. What is it about the country’s health system that has provoked the battles surrounding first Charlie, then Alfie, and now Alta?
The recent pleas for Alta’s transfer hold a note of disbelief: that a family with no UK citizenship could be prevented from taking their child for treatment abroad, at no cost to the state. That a hospital could effectively hold a patient prisoner. That a medical bureaucracy invested with the powers of life and death could deny parents the ultimate responsibility for deciding their child’s fate.
Now having lost their battle to take their case to Europe’s highest court, the Fixslers’ heartrending struggle appears bleak.
“We’re not public people, and this has been very hard on our lives,” says Avraham Fixsler with a weary note in his voice. “We feel like the UK is keeping us hostage. I’m not asking for money, just to let us go.”
“She’s a fighter”
Baby Alta’s tragedy began during a complicated birth in 2019 during which, for more than 25 minutes, she was starved of oxygen.
“Our oldest, a boy, was then five years old, and we’d been expecting a healthy baby,” says Avraham. “So after she was born, and they resuscitated her for 10 to 15 minutes, the doctor warned us that she wouldn’t live more than a few hours, and that we shouldn’t get too close to the baby.”
With a ventilator to help her breathe, the baby passed her first test when she survived those first few days — and evaded a medical classification that would have ended her chances of life.
“She’s a fighter, and she started to get a bit better,” says Avraham Fixsler. “But the doctors wanted to declare her brain-dead, which would have meant that all care could be withdrawn. I said, no, there’s a bit of movement. I had a feeling, and that was confirmed when they did some brain scans.”
It was in those early days that the Fixslers had an encounter that changed the mind of the senior doctor in the NICU. The doctor said that given the extent of the damage to her brain, the baby would have a very limited lifespan and poor quality of life.
“I told him, ‘The One Who chose to give her to us will decide when to take her.’ The doctor almost cried, and then said, ‘If this is what you want, we will try to do everything to help her.’ Two weeks later, that doctor told me, ‘Your words are still ringing in my ears.’ ”
The decision to fight on wasn’t one that the Fixslers took on their own. Rabbanim from Chayim Aruchim, an American Agudah-affiliated organization specializing in end-of-life issues, said that the parents should do everything they could to keep their child alive.
As a Belzer chassid, Avraham Fixsler traveled to Israel to consult his rebbe about whether subordinating family life — including their older child’s normal existence — to a round-the-clock battle to save the baby, was the correct course. The Belzer Rebbe encouraged him to go ahead, and named the baby “Alta” as a segulah for long life.
With the medical team on board, the improvement in the baby’s breathing continued until, at two months old, doctors in the NICU decided to wean her off the ventilator. That, the Fixslers were to find out, was the key test as far as the hospital was concerned. Ventilator-assisted breathing wasn’t a long-term option in a hospital — and there was no possibility of using a ventilator at home.
“I’m originally from the US and Israel,” says Avraham Fixsler, “and in both places there is specialized long-term care beyond hospitals. I discovered that in England there are hospices, but they’re only for end-of-life care for a few weeks, and they don’t use ventilators, only oxygen. There simply was no option for care outside the system.”
With the NICU specialist hopeful that Alta could be released, social services visited the Fixsler home to assess what long-term care would require. At the same time, the supportive doctor said that a tracheostomy was needed to facilitate Alta’s breathing with oxygen. That, it turned out, would require surgery in the children’s hospital — and a change in medical team.
“Here in the UK, the NICU is not part of the children’s hospital, and I was reluctant to lose this doctor who had been very supportive. I told him, ‘Promise me that they won’t move the baby until both sets of doctors have met with us to discuss Alta’s future.’ They promised, and so I left it.”
Broken Promises
It was one Motzaei Shabbos about a year ago that things started to go downhill. The Fixslers got an urgent phone call. “A nurse told us that Alta was about to be moved and that we should come. I protested that we’d been promised a meeting before that happened, but she said that she was just following instructions.”
Driving across the city to where the Manchester University hospital complex is located, Avraham Fixsler was shocked to see that things were worse than he’d feared. “When I arrived, she’d already been moved, and it was from an ICU to a regular ward for children who could communicate. Alta can’t cry, and she has no way of reacting if secretions get stuck when she’s breathing. That’s why she needs 24/7 care, and in this ward, the nurses only visit once an hour.”
Even at that stage, the Fixslers weren’t thinking in terms of legal redress. Instead, they hoped to work with the hospital to clarify things. That Monday, the Fixslers met the NICU doctor who, it turned out, had himself only been notified of Alta’s transfer a few minutes before.
The new medical staff sought to calm the parents, urging them to test the arrangements for a week. Avraham Fixsler’s response was that with the level of care, Alta would soon need to be reconnected to the ventilator — a prediction that didn’t take long to be proven true.
“About a week later, Covid had hit the UK and I got a call. ‘Come quick, Alta’s not breathing — it could be Covid.’ I responded that it wasn’t Covid that was at fault, but simply the lower standards of care.”
Alta was reconnected to the ventilator, and when the Covid tests came back negative, the doctors told the Fixslers that this time, there was no hope of weaning her off. It was time to talk of different ways of dealing with her condition, since going home wasn’t an option.
“I understood what they were referring to,” says Avraham Fixsler, “so at the next meeting after Pesach, I told the doctors, ‘I’ll take her home and pay for a ventilator and nurses myself.’”
The medical team’s response was that home care wasn’t an option, and when the Fixslers demanded to know why, they were surprised to hear something new.
“Because she’s suffering pain,” they were told.
“That was the first time we’d heard that claim,” says Avraham Fixsler. “Sometimes Alta shakes her hand and head, but the NICU doctor said that it wasn’t pain, but a reflex. I’ve since gotten the opinion of other neurologists who confirm that there’s no pain, and this claim only appeared in the children’s hospital when they realized that she would have to stay permanently on a ventilator.”
The issue of when exactly the hospital raised the subject of Alta’s pain features in the High Court ruling of May this year. Justice Alistair MacDonald noted that “the parents contend that, initially, the possibility of Alta going home was discussed, at which time there was no mention of Alta being in pain. The NHS Trust contend that palliative care was discussed with the family from the outset and that pain has likewise been an issue for Alta from the beginning.”
But while the judge concluded that ongoing pain was the only standard by which to determine the case, the possibility that pain was never raised initially might suggest that the presence of pain itself is not clear cut, as indeed the ruling discusses at length.
And despite the court ruling, the evidence on pain is mixed. Writing in the London Times this week, Dominic Lawson quotes Dr. Rajesh Munglani, a leading authority on pain, as calling the judgment “fundamentally flawed.”
“The judge’s first point was that ‘suffering’ is a higher cognitive function, in which Alta is entirely deficient,” Dr. Munglani said. “His second point was that given her permanent lack of consciousness, to say she probably experiences pain is simply wrong. I have patients with total spinal injury who have spasms, but no pain, because the link between the nerves and the brain is lost. This is almost certainly true also of Alta Fixsler.”
All of that was the subtext to the opening of the legal battle in December 2020. Despite the building tension, the hospital management had been very professional in dealing with Alta’s case, but when the Fixslers rejected the option of palliative care, there was only one option left.
“You’ll need to get yourself a legal team,” they said, “because we’re going to court.”
“Just Let Us Go!”
For a measure of just how well-known the case has become, look no further than the British Guardian newspaper. When the ECHR’s decision was announced last week, the paper’s website, which has a global audience, headlined the update very simply. “Alta Fixsler,” it read, with no further identification details needed.
The case first made the headlines after the first court ruling back in May. Media outlets, both British and international, immediately drew comparisons to the cases of Charlie Gard and Alfie Evans, two similar high-profile struggles of parents to treat their British-born sick children outside of the UK.
Charlie’s case captured the news in 2017 when as an 11-month-old baby with a degenerative brain and muscle disease, his parents decided to seek experimental treatment in the US. British doctors felt that the treatment was not in the child’s best interests, given the amount of brain damage. A year later, Alfie Evans’s case hit the headlines. Alfie had a degenerative neurological condition, and the Liverpool hospital that was treating him said that continued life support was “unkind and inhumane.” A court denied the right of Alfie’s parents to transfer him for treatment in Italy. He was disconnected from life support and died a few days later.
Online funding and lobbying campaigns — which became known as “Alfie’s Army” and “Charlie’s Army” — exerted pressure on authorities to reverse both decisions. But despite high-profile interventions ranging from the Pope to President Trump, British authorities remained adamant then, as they have now in Alta’s case.
Avraham Fixsler says that despite the similarities, Alta’s case is more clear cut. “The difference is that none of us are British. We joined my in-laws, who are Israeli, in England in 2014. I’m American and Israeli, my wife is Israeli with Hungarian citizenship — none of us are British.”
That contention — that ultimately Alta belongs elsewhere — is at the heart of the political effort to bring her overseas.
An effective lobbying effort brought support from both Republican and Democratic senators in the US, and an appeal from Senate Majority Leader Chuck Schumer was couched in strong terms. In a statement, he said: “My heart breaks for the Fixsler family. We’ve got them US visas, and I’ve written to the British ambassador and asked why Alta can’t come if her father’s an American citizen. We’re going to keep fighting because her life is at stake. For some reason the UK is still not letting her go — it’s hard to figure out why.”

Value Judgments
Chuck Schumer’s imponderable — why Alta is being held in Britain against her parents’ wishes — is just one of several. He might wonder, as well, why this is the third such battle in recent years to come out of the UK.
David Foster, who currently represents the Fixslers, is a barrister who specializes in pro-life cases such as these, and he explains that there are a number of factors at work. “I’ve been doing these cases for a long time,” he says, “and they come in front of the courts every few months, but don’t get to the media. What’s different about the UK, as opposed to Israel or Germany, where I’ve worked with doctors, is that in those countries you’ll often hear doctors say, ‘I wouldn’t dream of withdrawing support.’ But in Britain, which has a more secular-liberal culture, doctors will make that decision.
“In America,” he adds, “they’re more advanced in giving adequate respect and space to those of a particular faith. And that’s where I think the court hasn’t given sufficient weight to the fact this is a chassidic family, unlike, say, the Charlie Gard case.”
But it’s not just the value judgments that worked against the Fixslers; the NHS’s very size is also a factor. As its name implies, the organization is a national-scale health provider — decisions are calibrated for their effect on the whole.
“In the US, you can have a diversity of opinion and outcomes,” Foster explains, “but since this is a national health service, decisions need to be consistent with those made everywhere. So when you get a case like this, there’s no option of going elsewhere. A national organization like the NHS lends itself to homogeneous outcomes, which can go against a minority approach.”
In Justice MacDonald’s High Court ruling, one statement that raised eyebrows was how to assess Alta’s “best interests.”
“I am not able to accept that the assessment of Alta’s perspective should start from the assumption that Alta would share the values of her parents,” wrote MacDonald. “I am satisfied that, in circumstances where she has not developed any understanding of the faith into which she was born, and giving due weight to the fact that a child’s attitude may be, and often is influenced by the views, beliefs and guidance of his or her parents, it is more likely than not that Alta’s point of view would be that continued life-sustaining treatment would not be acceptable to her.”
The idea that, in effect, being Jewish only starts when a child is old enough to understand her religion is new ground, according to Foster. But even to a lay observer, the precedent is potentially alarming. What, for example, prevents a judge from banning non-medical circumcision on the grounds that a baby is too young to have a religion?
In the vast accretion of British case law, it’s one more reason that Alta Fixsler is setting a worrying precedent.
Everyday Heartbreak
After almost ten months of legal battle, Avraham Fixsler looks back at the entrenched opinions of both sides.
“There’ve been times when we’ve been made to feel that we were doing the wrong thing for fighting for our daughter. In court, they claimed that we didn’t come to the hospital a lot, although we have a son who has to be looked after. They said that we only got clothes from charity, which is not true at all, but it was meant to show that we were just fighting because we felt we had to, but not because we cared for the child. Of course, that has an effect on the outcome of the case.”
And in retrospect, Avraham Fixsler thinks, there was another mistake. He’d wanted to go public earlier, but was advised by his then legal team that public pressure would be counterproductive.
“I think that was wrong,” Avraham says. “The fact that Chuck Schumer and other US senators arranged a visa and asked for her to be transferred made it a case of public interest, which is why the UK Supreme Court agreed to hear the appeal.”
In the wake of the European Human Rights Court’s decision not to hear the case, Schumer rushed out a new appeal to the British ambassador in Washington, asking as a “matter of life and death” to reconsider, “in light of the long US-UK alliance.” Although as David Foster says, this is a legal matter, where courts are free of political pressure, he concedes that the NHS’s refusal to consider treatment elsewhere may be informed by an element of pride.
“Trying to move children in these cases is essentially saying that the child will be better cared for elsewhere,” he says. And the UK wouldn’t publicly acknowledge that its national health system is subpar.
As the heartbreak over Alta Fixsler’s fate continues to capture media space, this little girl’s very name stands as a warning about end-of-life issues in a liberal medical system in which doctors’ assessments hold more weight than religious rights or parents’ own wishes.
With all the ink spilled over the tragic struggle of the parents for their sweet little girl, it was the London Times that put the case for humanity against the strict rules that have been applied again and again by the NHS.
“Let Alta Fixsler go,” wrote Dominic Lawson, “to end her life with her extended family, rather than at a time of the British state’s choosing, in a windowless room in Royal Manchester Children’s Hospital.”
Give the Parents a Say
Just like the cases of Alfie Evans and Charlie Gard before her, the tragic struggle to take Alta Fixsler beyond UK shores for treatment has seemingly hit an immovable legal wall. But an effort to prevent cases like these from appearing in British courts is underway. “Charlie’s Law,” a push by Charlie Gard’s parents — who lead a foundation in their son’s memory — to redefine the law to give parents more of a say, has made it to Parliament.
The proposed amendment to the 1998 Human Rights Act — a law that provides for a “best interests” assessment for a person who is incapacitated — would ask instead whether a parent’s choice would cause significant harm to the child.
Alongside the ongoing expensive legal battle, askanim who’ve helped the Fixslers are exploring a way to join this effort, both for Britain’s Jewish community and for all British children. They propose a full-service organization that will enable children in similar situations to be transferred for treatment elsewhere.
(Originally featured in Mishpacha, Issue 873)
Oops! We could not locate your form.













